
Multe femei au dureri ovariene de-a lungul vieții lor. Dacă te-ai confruntat vreodată cu asta, e normal să te îngrijorezi. Și ca să te ajutăm să înțelegi ce este și ce trebuie să faci, ți-am pregătit un articol plin de informații utile, atunci când ai dureri de ovare.
Principalele cauze posibile pentru durerea de ovare
Un prim lucru pe care al trebui să-l știi este că durerea de ovare nu este întotdeauna ce pare. Practic, este o durere în zona abdominală, și doar în urma unui consult ginecologic poți afla dacă într-adevăr ai o problemă la nivelul ovarelor, sau dacă durerea este localizată și provine dintr-o afecțiune a altor organe.
Dacă totuși ovarele sunt cele care îți provoacă durere, cauzele pot varia de la afecțiuni grave, până la motive ce nu sunt îngrijorătoare. Principalele surse ale durerii sunt:
- Durerea la ovulație (mittelschmerz)
- Menstruația
- Chisturile ovariene
- Endometrioza
- Boala inflamatorie pelvină (anexita)
- Tumorile ovariene
- Cancerul ovarian
- Torsiunea ovariană
- Sindromul ovarian remanent
Ovulatie dureroasa
Ovulația dureroasă, sau ovulagia, este durerea de ovare care apare în timpul ovulației și cu care se confruntă aproximativ 20% dintre femei. Se poate simți ca o durere ascuțită (ca un junghi), sau ca un spasm ușor, în regiunea pelvină sau în partea inferioară a abdomenului.
Te întrebi cum apare durerea? Ei bine, pe măsură ce membrana care acoperă ovulul se întinde pentru ca acesta să fie eliberat de ovar, întinderea aceea provoacă presiune și durere. De obicei, este mai intensă pe o parte – cea pe care ovarul eliberează un ovul.
Rareori durerea poate dura câteva zile și poate fi insuportabilă, dar de cele mai multe ori este vorba doar despre un disconfort minor și de scurtă durată.
Inainte si in timpul menstruatiei
Unele femei simt durere în zona ovarelor înainte să le vină menstruația, sau în timpul menstrei. La fel ca în cazul durerii la ovulație, nu este o durere îngrijorătoare și în general dispare la câteva zile după debutul sângerării menstruale.
Termenul potrivit în acest caz, și cel pe care îl folosesc majoritatea femeilor pentru a descrie acest tip de durere, este de “crampe menstruale”. Ele sunt normale atâta timp cât nu te împiedică să-ți desfășori activitățile zilnice, și apar când uterul se contractă pentru a stimula eliminarea mucoasei uterine și a sângelui menstrual. Plasturii termici pot ajuta la ameliorarea acestor dureri.
Dureri ovare in afara menstruatiei
Pentru durerile de ovare în afara menstruației, cauzele sunt mult mai numeroase și variate, și nu la fel de inofensive precum crampele din timpul menstruației. Motivele pot fi de la afecțiuni ginecologice până la alte probleme de sănătate, inclusiv apendicita.
Câteva afecțiuni frecvente care îți pot provoca dureri de ovare în afara menstruației sunt chisturile, endometrioza și anumite infecții sau boli cu transmitere sexuală. Boala inflamatorie pelvină, care este o inflamație a organelor reproductive interne (ovare, trompe uterine, uter și cervix), poate fi de asemenea sursa durerilor de ovare chiar dacă nu ești la menstruație. La fel și torsiunea ovariană, respectiv când ovarul se răsucește în jurul ligamentului de care e atașat.
Acestea sunt afecțiuni care necesită tratament și, drept urmare, nu ar trebui ignorate. Nu considera normale durerile de ovare în afara menstruației, și programează întotdeauna o vizită la medicul specialist pentru diagnostic și tratament, în special dacă simptomele se intensifică sau persistă mai multe zile.
Un chist ovarian
Formațiunile cu lichid care apar pe ovare se numesc chisturi ovariene, și se numără printre cele mai frecvente cauze ale durerilor de ovare. Deși pot trece neobservate timp îndelungat fără să provoace disconfort, chisturile își pot face simțită prezența prin simptome precum durerea (care se poate extinde înspre picior sau spate, și care apare în timpul contactului sexual sau la menstruație), sângerările vaginale neobișnuite, presiune la nivelul vezicii urinare și mărirea abdomenului.
De multe ori pot să dispară de la sine, fără tratament, după puțin timp. Dar există și cazuri când medicul poate recomanda un tratament cu anticoncepționale pentru prevenția chisturilor, sau îndepărtarea chirurgicală când chisturile provoacă disconfort continuu. Dacă vrei să afli mai multe despre această afecțiune, ți-am explicat totul AICI.
Dupa actul sexual
Chisturile ovariene și endometrioza se numără printre afecțiunile ginecologice care provoacă frecvent dureri de ovare ce se intensifică mai ales după actul sexual, dar nu sunt singurele.
O altă cauză importantă pentru acest tip de durere o constituie boala inflamatorie pelvină, care poate fi provocată de mai multe bacterii și mai ales de infecții cu transmitere sexuală precum gonoreea și chlamydia, dar și altele despre care ți-am povestit mai multe AICI. Și cancerul ovarian poate fi o cauză a durerilor de ovare după actul sexual.
Durerea de ovare poate fi totodată de natură anatomică, spre exemplu atunci când apare doar la finalul actului sexual. Cauza este, atunci, nu la nivelul ovarului, ci al unui uter retrovers, care provoacă “lovirea” dureroasă a penisului de colul uterin în timpul contactului sexual.
O infectie
Nu ne referim aici la infecțiile vaginale, despre care poți citi mai multe în articolul nostru. Durerea de ovare poate fi provocată de un abces la nivelul ovarului, de obicei la pacientele care suferă de o boală infecțioasă. Pe lângă infecțiile discutate deja mai sus, o altă infecție de acest tip este salpingita.
Aceasta apare când una sau ambele trompe uterine se infectează ca urmare a contactării unei infecții cu transmitere sexuală, a infectării unui organ din proximitatea aparatului reproducător (ex: apendicita), a introducerii unui sterilet sau a efectuării unui examen endouterin. O astfel de infecție este însoțită de febră și scurgeri neobișnuite, se diagnostichează doar de către medic cu ajutorul unei ecografii pelvine, și se tratează cu antibiotic.
Dupa fertilizare in vitro (FIV)
Fertilizarea in vitro este o procedură avansată de reproducere asistată recomandată în cazul infertilității, care constă în fertilizarea artificială și alegerea unuia sau a mai multor embrioni pentru a fi transferați în uter, cu scopul de a începe o sarcină sănătoasă.
Însă dacă o astfel de procedură solicită ovarele prea mult, spre exemplu dacă stimularea este foarte puternică, acest lucru poate provoca apariția chisturilor ovariene și a posibilelor dureri de ovare. Afecțiunea are chiar și o denumire – sindromul hiperstimulării ovariene (SHSO), și implică umflarea ovarelor și apariția durerii. Chisturile pot fi observate imediat de către medic, în cadrul unei ecografii.
9 afectiuni care pot ascunde durerea de ovare
Durere de Ovare la Ovulatie - Mittelschmerz
Durerea de ovare nu e ceva neobișnuit, dimpotrivă. Ea poate sa apară in perioada menstruației, însă nu numai: e comună și la ovulație, atunci când foliculul ovarian se rupe și este eliminat.
Simptome & diagnosticare Mittelschmerz
Deși este destul de comună, afecțiunea are un nume mai rar întâlnit: mittelschmerz. Numele provine de la cuvintele germane pentru "mijloc" și "durere".

Ovulația are loc, în general, la mijlocul ciclului menstrual, așa că este posibil să simțiți durerea cel mai mult în jurul zilei 14, în momentul în care ovulul izbucnește din ovar și ajunge în trompele uterine.
Diferite teorii explică de ce ovulația ar putea durea. O teorie este că, deoarece nu există o deschidere în ovar, ovulul trebuie să treacă prin peretele ovarului, ceea ce poate durea.
Durere de Ovare - Chist Ovarian
Atunci când durerea persistă și în afara menstruației sau ovulației, te poți confrunta cu un chist ovarian.
Chist Ovarian - Simptome & diagnosticare
Chistul ovarian apare sub forma unor săculeti rotunzi cu lichid, care se produc in urma unor modificări la ovulație. Aceste chisturi se pot rupe, răsuci sau sângera și pot cauza dureri extreme.
In marea majoritate a cazurilor, chisturile ovariene nu genereaza simptome si pot fi tratate medicamentos. In fazele acute ale bolii sau in momentul in care se rup sau se torsioneaza, este nevoie de tratament chirurgical. Dacă durerea de ovare persistă, este recomandat să mergi la un consult ginecologic, pentru diagnosticare.

Majoritatea chisturilor sunt asimptomatice și nu cauzează dureri sau complicații, însă unele din simptomele celor problematice pot fi durerea abdominală și nevoia de a urina mai des. Medicul îți poate recomanda tratament și ținerea sub observație a evoluției chisturilor. În cazuri rare, este necesară o intervenție minoră, laparoscopică, pentru a înlătura chisturile. Ginecologul îți mai poate recomanda și pilule anticoncepționale.
Durere de la Cancer Ovarian
Există mai multe tipuri de cancere ovariene care pot duce la durere ovariană, inclusiv cancerul ovarian epitelial, cancerul ovarian cu celule germinale, cancerul ovarian cu celule stromale și carcinomul cu celule mici. Deși toate sunt clasificate ca fiind "ovariene", deoarece privesc ovarele, acestea variază în ceea ce privește originea, tratamentul și diagnosticul.
Simptome & diagnostic Cancer Ovarian
Simptomele cancerului ovarian pot include:
- Durere de ovare severă sau mai persistentă decât disconfortul asociat cu un ciclu menstrual
- Balonare
- Dureri pelviene sau abdominale
- Dificultate în a mânca sau senzație de sațietate rapidă
- Simptome urinare (urgență sau frecvență)
Un ginecolog te poate ajuta să determini cauzele durerii și să stabilească un diagnostic.
Durerea de ovare - Endometrioza
Frecventă în rândul femeilor cu vârste între 25-35 de ani, endometrioza e cauza cea mai comună a durerilor pelvine cronice. Dar ce este boala, mai exact?

Endometrioza e o afecțiune cronică în care țesutul care căptușește uterul (endometrul) și fragmente de țesut asemănătoare se găsesc în afara uterului. Fragmentele de țesut se numesc și „leziuni de endometrioză” și au dimensiuni diferite; se găsesc în interiorul cavității abdominale și se pot răspândi pe parcursul unui ciclu menstrual.
Endometrioza - Simptome & diagnostic
Persoanele care suferă de endometrioză descriu durerea ca fiind mai puternică decât în mod obișnuit. Mai mult, cu timpul, durerea se poate agrava și se poate manifesta și la contactul sexual, care va fi dureros. Când spunem durere mai puternică, includem și imobilizarea la pat și durerile acute între menstre.
Simptomele includ, așadar:
- Dismenoreea - sau menstrele dureroase - când durerea și crampele sunt însoțite și de durere lombară și abdominală, și se poate extinde înainte și după menstră.
- Durerea în timpul contactului sexual
- Durerea abdominală în timpul urinării și/sau când stai pe toaletă
- Sângerare abundentă și sângerări între menstre
- Infertilitate
- Oboseală, diaree, greață, diaree și alte simptome
Boala Inflamatorie Pelvina (BIP)
Boala inflamatorie pelvină (BIP) este o infecție a organelor genitale la persoanele cu ovare. Aceasta poate afecta colul uterin, uterul, trompele uterine și ovarele și poate fi transmisă pe cale sexuală – însă nu este o regulă. În unele cazuri, BIP poate duce la afectarea permanentă a organelor genitale și la complicații grave, cum ar fi infertilitatea și riscul unei sarcini ectopice.
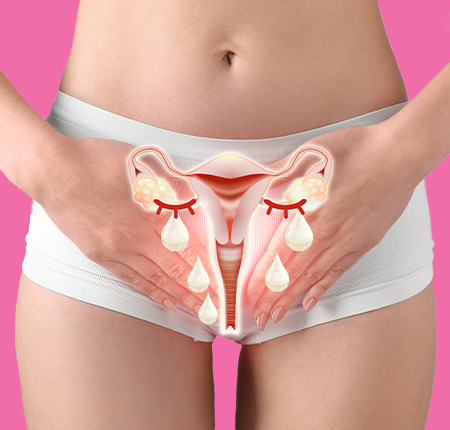
Simptome & diagnostic Boala Inflamatorie Pelvina
Cea mai frecventă manifestare și simptom al bolii inflamatorii pelvine este durerea de ovare, care poate deveni aproape permanentă. Însă nu e exclus să ai BIP fără simptome sau cu simptome care se confundă cu alte afecțiuni, precum:
- arsuri în timpul urinării
- urinare frecventă
- menstruații neregulate
- modificări ale secrețiilor vaginale
- durere în timpul sexului
- febră, cu sau fără frisoane
Mai mult, dacă porți un sterilet ca metodă de contracepție acesta poate, de asemenea, să cauzeze dureri.
Pentru diagnostic, este important să consulți medicul iar în urma unor teste vei afla ce a declanșat afecțiunea, pentru a primi tratamentul corespunzător.
Durerea provocata de torsiune ovariana
Torsiunea ovariană se întâmplă atunci când un ovar se răsucește în jurul ligamentelor care îl țin la locul său. Acest lucru poate întrerupe alimentarea cu sânge a ovarului și poate provoca moartea țesutului ovarian. Cel mai adesea, torsiunea ovariană se întâmplă din cauza unei mase pe ovar, cauzată de:
- un chist ovarian
- sindromul ovarului polichistic
- o tumoare pe ovar
Sarcina sau tratamentele de fertilitate sunt, de asemenea, factori de risc pentru torsiunea ovariană. Studii recente arată că între 8 - 15% din persoanele diagnosticate cu torsiune ovariană erau însărcinate.
Simptome & diagnostic Torsiune Ovariana
Simptomele de torsiune ovariană pot include:
- durere pelvină bruscă, severă, care poate iradia în abdomen, spate sau lateral
- Greață, vărsături
De asemenea, este posibil să aveți simptome care apar și dispar în decurs de câteva zile sau săptămâni. Diagnosticul de torsiune ovariană va implica analize de laborator de sânge și urină pentru a ajuta la excluderea altor afecțiuni și, la recomandarea medicului, ecografie și/sau test de sarcină.
Sindromul restului ovarian (SRO)
Sindromul restului ovarian este prezența țesutului ovarian rezidual după ce o femeie a suferit o intervenție chirurgicală pentru îndepărtarea unui ovar sau a ambelor ovare.
Simptome & diagnostic Sindromul restului ovarian
Semnele și simptomele sindromului restului ovarian pot include durere pelvină, o masă pelvină sau absența menopauzei după intervenția chirurgicală. Mai mult, poți avea simptome asemănătoare endometriozei, cum ar fi durere în timpul sexului, durere în timpul urinării sau al scaunului sau simptome digestive.
Pentru a diagnostica SRO, medicul tău va nota istoricul intervențiilor chirurgicale anterioare asupra ovarelor și îți va recomanda o ecografie. Diagnosticticul definitiv se face prin laparoscopie.
Durerile de ovare in timpul sarcinii
Durerea de ovare poate fi și unul din primele semne că ești însărcinată. Un semn de sarcină poate fi balonarea, pe lângă problemele digestive precum constipația și crampele abdominale. Atunci când rămâi însărcinată, nivelul de progesteron crește și poate cauza încetinirea digestiei, ceea ce duce la constipație. Crampele abdominale și durerea de ovare pot apărea însă, și în cazul menstruației, așa că e recomandat să faci un test de sarcină dacă nu ești sigură!
Durerea de ovare de la sarcina extrauterina (ectopica)
Dacă durerea de ovare este observată în același timp cu o întârziere a menstruației la o femeie aflată la vârsta fertilă, sarcina ectopică localizată la nivelul ovarului poate fi o cauză plauzibilă. Nu este o situație obișnuită, însă este posibilă.
Sarcina extrauterină are loc atunci când embrionul se implantează în afara uterului și, deși de cele mai multe ori se formează în trompele uterine, există și cazuri rare când se formează în cavitatea abdominală sau pe un ovar.
Dacă ai avut contact sexual neprotejat, ai uitat să iei o pilulă contraceptivă sau există orice posibilitate să fii însărcinată, se recomandă efectuarea unui test de sarcină. În cazul unui rezultat pozitiv, va trebui să te programezi pentru o ecografie. O sarcină extrauterină nu poate fi dusă la termen și poate ajunge la complicații ce îți pun sănătatea în pericol, așa că va trebui să discuți cu medicul specialist pașii următori.
Simptome & diagnosticare pentru durerea de la sarcina ectopica
Simptomele sarcinii ectopice pot fi foarte asemănătoare cu cele ale unei sarcini normale, în ceea ce privește primele semne. Îți întârzie menstruația, te simți mai obosită și ai senzația de slăbiciune, apare sensibilitatea crescută, sau începi să simți dureri puternice la nivelul ovarelor și observi sângerări vaginale neobișnuite.
De obicei, medicul ginecolog poate diagnostica durerea de ovare în timpul examinării fizice, prin palpare. Dar pentru a detecta sarcina ectopică, va fi nevoie de o ecografie. De obicei acest tip de sarcină este diagnosticat timpuriu, încă din primele 12 săptămâni, urmând să fie luate măsuri cât mai curând pentru a evita complicațiile ulterioare.
Ce este durerea referita de ovare - legatura cu alte afectiuni
Ovarele sunt situate în apropierea altor organe și părți ale corpului tău, așadar,poți avea dureri pelviene și ovariene cauzate de alte afecțiuni medicale. Spre exemplu, dacă ai dureri într-o parte a corpului care se datorează de fapt unei dureri într-o altă zonă, se numește durere referită.
Simptome & diagnosticare pentru Durerea Referita
Medicii încă încearcă să își dea seama de ce anume se întâmplă durerea referită! Este probabil ca durerea referită să apară din cauza modului în care nervii sunt conectați în corpul tău. O senzație de durere resimțită într-o zonă trebuie să ajungă la creier prin rețeaua de nervi, iar atunci când acești nervi se suprapun, pot cauza durere în altă locație.
Metode de tratament si remedii pentru durerea de ovare
Deși nu există un singur tratament și depinde de la persoană la persoană ce remedii pentru durerea de ovare funcționează (la fel cum diferă și intensitatea crampelor), poți încerca câteva metode naturale de tratament atunci când durerea de ovare te bâzâie.
Deși nu există un singur tratament iar remediile care funcționează depind de la persoană la persoană (și intensitatea crampelor), poți încerca câteva metode naturale de tratament atunci când durerea de ovare te bâzâie.
Recomandările noastre pentru ameliorarea crampelor:
- Plasturii naturali menstruali: lipește plasturele unde te doare și bucură-te de până la 8 ore fără crampe!
- Analgezice și antiinflamatoare: dacă nu poți ameliora crampele în mod natural, găsești la farmacie medicamente speciale pentru durerile menstruale.
- Evitarea consumului excesiv de sare, zahăr, carne roșie, alcool: acestea pot provoca balonare, care îți poate intensifica durerile.
- Hidratarea corespunzătoare: consumă suficiente lichide și electroliți.
- Suplimentele alimentare sau creșterea consumului de fructe, legume, nuci și semințe pentru vitamine și minerale: dieta echilibrată se numără printre cele mai simple și naturale remedii pentru durerea de ovare, fiindcă durerile se pot ameliora când corpul nu are deficiențe nutriționale și este echilibrat hormonal.
- Analgezice și antiinflamatoare
- Evitarea consumului excesiv de sare, zahăr, carne roșie, alcool
- Hidratarea corespunzătoare
- Suplimentele alimentare sau creșterea consumului de fructe, legume, nuci și semințe pentru vitamine și minerale.
Cand trebuie sa te duci la medic?
Dacă ai și alte simptome în afară de durerea de ovare sau bănuiești o afecțiune cum sunt cele de mai sus despre care am scris în articol, îți recomandăm să consulți un medic neapărat. Pentru că tratamentele pot fi diferite: boala inflamatorie pelvină poate necesita antibiotice, iar torsiunea de ovare este o urgență medicală!
Nu în ultimul rând, pentru că durerea de ovare și dismenoreea sunt în strânsă legătură cu sindromul premenstrual, îți recomandăm articolul nostru despre tot ce înseamnă SPM: ce este, care sunt simptomele fizice și emoționale, cum îți influențează sănătatea, care sunt cauzele și factorii de risc.
Intrebari frecvente legate de durerea de ovare
Dacă mai ai și alte întrebări cu privire la durerea de ovare, verifică secțiunea de întrebări frecvente. Încercăm să-ți oferim aici răspunsuri concise și clare privind toate întrebările pentru care poate că nu ai găsit încă răspunsul în articol.
De ce te dor ovarele dupa contact sexual?
Există mai multe cauze posibile pentru durerile de ovare după un contact sexual. Printre cele mai comune se numără bolile cu transmitere sexuală, chisturile ovariene, dar și structura uterului.
În cazul bolilor cu transmitere sexuală, inflamarea organelor interne poate provoca dureri și sângerări după actul sexual. În cazul chisturilor ovariene, ele pot fi asimptomatice până în momentul în care se rup. Astfel, este posibil ca durerea după contact să indice ruperea chistului. Iar în ultima situație, poziționarea retroversă a uterului (în condițiile în care poziția normală este cea anteversă) poate fi motivul pentru care penisul atinge în mod repetat colul uterin, provocând astfel durere la finalul actului sexual.
Durerea de ovare se lasa pe picior?
Da, este posibil ca durerea localizată la nivelul ovarelor și al abdomenului inferior să iradieze spre picior sau spre spate. De obicei, cauza este fie o problemă de sănătate precum apendicita, fie o problemă ginecologică precum chistul ovarian. Acesta poate intensifică durerile mai ales în timpul menstruației sau în timpul/după un contact sexual.
Dacă te confrunți cu astfel de simptome, nu le ignora. Programează o vizită la medicul ginecolog pentru a determina cauza exactă și a stabili următorii pași. Unele chisturi trec de la sine fără tratament, pe când altele au nevoie de intervenție chirurgicală pentru a elimina disconfortul.
La durerea de ovare tratamentul naturist e eficient?
Dacă vorbim despre durerile pe care le simți în timpul menstruației, cu siguranță poți încerca remedii naturale pentru ameliorarea lor. Atâta timp cât au un nivel suportabil, crampele menstruale sunt normale și poți scăpa eficient de ele folosind plasturii menstruali de la Enroush cu ingrediente 100% naturale, care folosesc terapia prin căldură pentru a te ajuta să te relaxezi, fără medicamente.
În schimb, dacă durerea apare în afara menstruației sau ai motive să crezi că e provocată de alte afecțiuni, întotdeauna se recomandă vizita la medicul ginecolog pentru diagnostic și tratament eficient. Iar dacă îți dorești să urmezi un tratament naturist, discută acest lucru cu medicul tău și urmează-i sfaturile.
Durerea de ovare si spate este normala in perioada ovulatiei?
Durerea de ovare (care se poate întinde până la nivelul spatelui) nu este atât de neobișnuită la ovulație. Da, ovulațiile dureroase pot fi normale și în general nu reprezintă un motiv de îngrijorare sau o afecțiune gravă, și nici nu îți afectează fertilitatea.
Ele apar din cauză că membrana care acoperă ovulul se întinde pentru ca acesta să fie eliminat, astfel punând presiune și provocând durere. De asemenea, sângele eliminat la împingerea ovulului poate irita mucoasa abdominală, accentuând durerea.
Totuși, dacă disconfortul devine foarte puternic, persistă multe zile sau apar și alte simptome, nu ar trebui să normalizăm acest lucru.
Surse
Pentru realizarea acestui articol, am consultat informații din următoarele surse:
1. NIH, National Library of Medicine, “Ovarian Conditions As Causes Of Pelvic Pain”: https://pmc.ncbi.nlm.nih.gov/articles/PMC2445661/
2. Cleveland Clinic, “Ovary Pain”: https://my.clevelandclinic.org/health/symptoms/24726-ovary-pain
3. Healthline, “Causes and Treatments for Ovary Pain”: https://www.healthline.com/health/womens-health/ovary-pain
4. WebMD, “Ovarian Pain: Possible Causes, Diagnosis, and Treatments”: https://www.webmd.com/women/ovarian-pain-causes-diagnosis-treatments
5. Ovarian Cancer Research Alliance, “5 Possible Causes for Ovary Pain”: https://ocrahope.org/news/5-possible-causes-for-ovary-pain/
6. VeryWell Health, “12 Possible Causes of Ovary Pain and Treatment Options”: https://www.verywellhealth.com/ovary-pain-causes-and-treatment-514437
7. Mayo Clinic, “Ovarian cysts”: https://www.mayoclinic.org/diseases-conditions/ovarian-cysts/symptoms-causes/syc-20353405
8. Mayo Clinic, “Ovary hyperstimulation syndrome”: https://www.mayoclinic.org/diseases-conditions/ovarian-hyperstimulation-syndrome-ohss/symptoms-causes/syc-20354697
9. Mayo Clinic, “Ectopic pregnancy”: https://www.mayoclinic.org/diseases-conditions/ectopic-pregnancy/diagnosis-treatment/drc-20372093























